Search
- Page Path
- HOME > Search
- Thyroid
- The Early Changes in Thyroid-Stimulating Immunoglobulin Bioassay over Anti-Thyroid Drug Treatment Could Predict Prognosis of Graves’ Disease
- Jin Yu, Han-Sang Baek, Chaiho Jeong, Kwanhoon Jo, Jeongmin Lee, Jeonghoon Ha, Min Hee Kim, Jungmin Lee, Dong-Jun Lim
- Endocrinol Metab. 2023;38(3):338-346. Published online June 9, 2023
- DOI: https://doi.org/10.3803/EnM.2023.1664

- 1,789 View
- 102 Download
- 1 Web of Science
- 2 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub - Background
To determine whether baseline thyroid-stimulating immunoglobulin (TSI) bioassay or its early response upon treatment with an anti-thyroid drug (ATD) can predict prognosis of Graves’ disease (GD) in real-world practice.
Methods
This retrospective study enrolled GD patients who had previous ATD treatment with TSI bioassay checked at baseline and at follow-up from April 2010 to November 2019 in one referral hospital. The study population were divided into two groups: patients who experienced relapse or continued ATD (relapse/persistence), and patients who experienced no relapse after ATD discontinuation (remission). The slope and area under the curve at 1st year (AUC1yr) of thyroid-stimulating hormone receptor antibodies including TSI bioassay and thyrotropin-binding inhibitory immunoglobulin (TBII) were calculated as differences between baseline and second values divided by time duration (year).
Results
Among enrolled 156 study subjects, 74 (47.4%) had relapse/persistence. Baseline TSI bioassay values did not show significant differences between the two groups. However, the relapse/persistence group showed less decremental TSI bioassay in response to ATD than the remission group (–84.7 [TSI slope, –198.2 to 8.2] vs. –120.1 [TSI slope, –204.4 to –45.9], P=0.026), whereas the TBII slope was not significantly different between the two groups. The relapse/persistence group showed higher AUC1yr of TSI bioassay and TBII in the 1st year during ATD treatment than the remission group (AUC1yr for TSI bioassay, P=0.0125; AUC1yr for TBII,P =0.001).
Conclusion
Early changes in TSI bioassay can better predict prognosis of GD than TBII. Measurement of TSI bioassay at beginning and follow-up could help predict GD prognosis. -
Citations
Citations to this article as recorded by- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study
Xinpan Wang, Tiantian Li, Yue Li, Qiuyi Wang, Yun Cai, Zhixiao Wang, Yun Shi, Tao Yang, Xuqin Zheng
Journal of Translational Medicine.2024;[Epub] CrossRef - Long-term Effect of Thyrotropin-binding Inhibitor Immunoglobulin on Atrial Fibrillation in Euthyroid Patients
Jung-Chi Hsu, Kang-Chih Fan, Ting-Chuan Wang, Shu-Lin Chuang, Ying-Ting Chao, Ting-Tse Lin, Kuan-Chih Huang, Lian-Yu Lin, Lung-Chun Lin
Endocrine Practice.2024;[Epub] CrossRef
- Enhanced predictive validity of integrative models for refractory hyperthyroidism considering baseline and early therapy characteristics: a prospective cohort study

- Diabetes, Obesity and Metabolism
Big Data Articles (National Health Insurance Service Database) - Predicting the Risk of Insulin-Requiring Gestational Diabetes before Pregnancy: A Model Generated from a Nationwide Population-Based Cohort Study in Korea
- Seung-Hwan Lee, Jin Yu, Kyungdo Han, Seung Woo Lee, Sang Youn You, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim
- Endocrinol Metab. 2023;38(1):129-138. Published online January 27, 2023
- DOI: https://doi.org/10.3803/EnM.2022.1609

- 2,188 View
- 157 Download
- 5 Web of Science
- 5 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The severity of gestational diabetes mellitus (GDM) is associated with adverse pregnancy outcomes. We aimed to generate a risk model for predicting insulin-requiring GDM before pregnancy in Korean women.
Methods
A total of 417,210 women who received a health examination within 52 weeks before pregnancy and delivered between 2011 and 2015 were recruited from the Korean National Health Insurance database. The risk prediction model was created using a sample of 70% of the participants, while the remaining 30% were used for internal validation. Risk scores were assigned based on the hazard ratios for each risk factor in the multivariable Cox proportional hazards regression model. Six risk variables were selected, and a risk nomogram was created to estimate the risk of insulin-requiring GDM.
Results
A total of 2,891 (0.69%) women developed insulin-requiring GDM. Age, body mass index (BMI), current smoking, fasting blood glucose (FBG), total cholesterol, and γ-glutamyl transferase were significant risk factors for insulin-requiring GDM and were incorporated into the risk model. Among the variables, old age, high BMI, and high FBG level were the main contributors to an increased risk of insulin-requiring GDM. The concordance index of the risk model for predicting insulin-requiring GDM was 0.783 (95% confidence interval, 0.766 to 0.799). The validation cohort’s incidence rates for insulin-requiring GDM were consistent with the risk model’s predictions.
Conclusion
A novel risk engine was generated to predict insulin-requiring GDM among Korean women. This model may provide helpful information for identifying high-risk women and enhancing prepregnancy care. -
Citations
Citations to this article as recorded by- Establishment and validation of a nomogram to predict the neck contracture after skin grafting in burn patients: A multicentre cohort study
Rui Li, Yangyang Zheng, Xijuan Fan, Zilong Cao, Qiang Yue, Jincai Fan, Cheng Gan, Hu Jiao, Liqiang Liu
International Wound Journal.2023; 20(9): 3648. CrossRef - Predicting the Need for Insulin Treatment: A Risk-Based Approach to the Management of Women with Gestational Diabetes Mellitus
Anna S. Koefoed, H. David McIntyre, Kristen S. Gibbons, Charlotte W. Poulsen, Jens Fuglsang, Per G. Ovesen
Reproductive Medicine.2023; 4(3): 133. CrossRef - Prepregnancy Glucose Levels Within Normal Range and Its Impact on Obstetric Complications in Subsequent Pregnancy: A Population Cohort Study
Ho Yeon Kim, Ki Hoon Ahn, Geum Joon Cho, Soon-Cheol Hong, Min-Jeong Oh, Hai-Joong Kim
Journal of Korean Medical Science.2023;[Epub] CrossRef - Risk of Cause-Specific Mortality across Glucose Spectrum in Elderly People: A Nationwide Population-Based Cohort Study
Joonyub Lee, Hun-Sung Kim, Kee-Ho Song, Soon Jib Yoo, Kyungdo Han, Seung-Hwan Lee
Endocrinology and Metabolism.2023; 38(5): 525. CrossRef - The CHANGED Score—A New Tool for the Prediction of Insulin Dependency in Gestational Diabetes
Paul Rostin, Selina Balke, Dorota Sroka, Laura Fangmann, Petra Weid, Wolfgang Henrich, Josefine Theresia Königbauer
Journal of Clinical Medicine.2023; 12(22): 7169. CrossRef
- Establishment and validation of a nomogram to predict the neck contracture after skin grafting in burn patients: A multicentre cohort study

- Diabetes, Obesity and Metabolism
- Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
- Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
- Endocrinol Metab. 2022;37(6):945-946. Published online December 2, 2022
- DOI: https://doi.org/10.3803/EnM.2022.602
- [Original]
- 1,766 View
- 165 Download

- Calcium & Bone Metabolism
- Update on Preoperative Parathyroid Localization in Primary Hyperparathyroidism
- Hye-Sun Park, Namki Hong, Jong Ju Jeong, Mijin Yun, Yumie Rhee
- Endocrinol Metab. 2022;37(5):744-755. Published online October 25, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1589

- 4,130 View
- 357 Download
- 5 Web of Science
- 6 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Parathyroidectomy is the treatment of choice for primary hyperparathyroidism when the clinical criteria are met. Although bilateral neck exploration is traditionally the standard method for surgery, minimally invasive parathyroidectomy (MIP), or focused parathyroidectomy, has been widely accepted with comparable curative outcomes. For successful MIP, accurate preoperative localization of parathyroid lesions is essential. However, no consensus exists on the optimal approach for localization. Currently, ultrasonography and technetium-99m-sestamibi–single photon emission computed tomography/computed tomography are widely accepted in most cases. However, exact localization cannot always be achieved, especially in cases with multiglandular disease, ectopic glands, recurrent disease, and normocalcemic primary hyperparathyroidism. Therefore, new modalities for preoperative localization have been developed and evaluated. Positron emission tomography/computed tomography and parathyroid venous sampling have demonstrated improvements in sensitivity and accuracy. Both anatomical and functional information can be obtained by combining these methods. As each approach has its advantages and disadvantages, the localization study should be deliberately chosen based on each patient’s clinical profile, costs, radiation exposure, and the availability of experienced experts. In this review, we summarize various methods for the localization of hyperfunctioning parathyroid tissues in primary hyperparathyroidism.
-
Citations
Citations to this article as recorded by- Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue
Anne L. Worth, Mesrop Ayrapetyan, Susan J. Maygarden, Zibo Li, Zhanhong Wu, Chris B. Agala, Lawrence T. Kim
Journal of Surgical Research.2024; 293: 618. CrossRef - Use of [18F]fluorocholine PET/CT in the detection of primary hyperparathyroidism in paediatrics: a case report
Helena Martínez Sánchez, Francisca Moreno Macián, Sara León Cariñena, Carmen de Mingo Alemany, Lidia Blasco González, Raquel Sánchez Vañó
Journal of Pediatric Endocrinology and Metabolism.2024;[Epub] CrossRef - A Rare Case of Hyperfunctioning Lipoadenoma Presenting as a Cystic Pararthyroid Lesion
Jinyoung Kim, Ohjoon Kwon, Tae-Jung Kim, So Lyung Jung, Eun Ji Han, Ki-Ho Song
Journal of Bone Metabolism.2023; 30(2): 201. CrossRef - Role of 18F-Fluorocholine Positron Emission Tomography (PET)/Computed Tomography (CT) in Diagnosis of Elusive Parathyroid Adenoma
Janan R Badier, Pokhraj P Suthar, Jagadeesh S Singh, Miral D Jhaveri
Cureus.2023;[Epub] CrossRef - Pitfalls of DualTracer 99m-Technetium (Tc) Pertechnetate and Sestamibi Scintigraphy before Parathyroidectomy: Between Primary-Hyperparathyroidism-Associated Parathyroid Tumour and Ectopic Thyroid Tissue
Mara Carsote, Mihaela Stanciu, Florina Ligia Popa, Oana-Claudia Sima, Eugenia Petrova, Anca-Pati Cucu, Claudiu Nistor
Medicina.2023; 60(1): 15. CrossRef - Diagnostic Performance of Magnetic Resonance Imaging for Parathyroid Localization of Primary Hyperparathyroidism: A Systematic Review
Max H. M. C. Scheepers, Zaid Al-Difaie, Lloyd Brandts, Andrea Peeters, Bjorn Winkens, Mahdi Al-Taher, Sanne M. E. Engelen, Tim Lubbers, Bas Havekes, Nicole D. Bouvy, Alida A. Postma
Diagnostics.2023; 14(1): 25. CrossRef
- Expression of the Calcium-Sensing Receptor on Normal and Abnormal Parathyroid and Thyroid Tissue

- Diabetes, Obesity and Metabolism
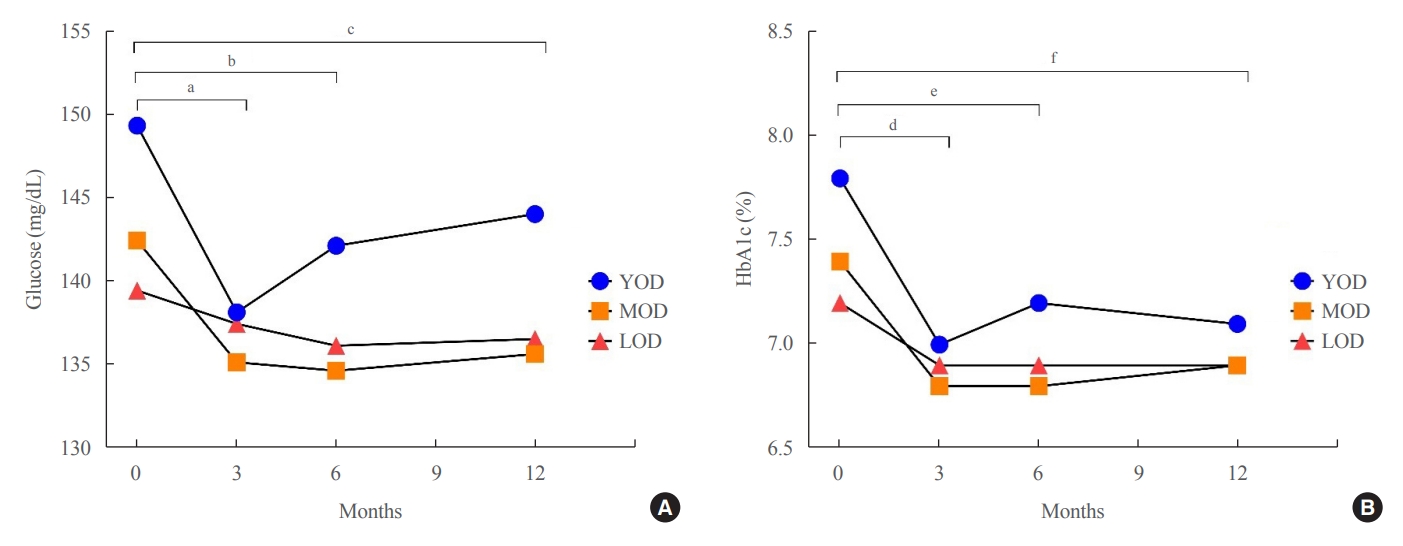
- Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes
- Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
- Endocrinol Metab. 2022;37(4):641-651. Published online August 29, 2022
- DOI: https://doi.org/10.3803/EnM.2022.1501
- 6,234 View
- 166 Download
- 10 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
The prevalence of young-onset diabetes (YOD) has been increasing worldwide. As the incidence of YOD increases, it is necessary to determine the characteristics of YOD and the factors that influence its development and associated complications.
Methods
In this retrospective study, we recruited patients who were diagnosed with type 2 diabetes mellitus between June 2001 and December 2021 at a tertiary hospital. The study population was categorized according to age: YOD (age <40 years), middle-age-onset diabetes (MOD, 40≤ age <65 years), and late-onset diabetes (LOD, age ≥65 years). We examined trends in glycemic control by analyzing fasting glucose levels during the first year in each age group. A Cox proportional-hazards model was used to determine the relative risk of developing complications according to glycemic control trends.
Results
The fasting glucose level at the time of diagnosis was highest in the YOD group (YOD 149±65 mg/dL; MOD 143±54 mg/dL; and LOD 140±55 mg/dL; p=0.009). In the YOD group, glucose levels decreased at 3 months, but increased by 12 months. YOD patients and those with poor glycemic control in the first year were at a higher risk of developing complications, whereas the risk in patients with LOD was not statistically significant.
Conclusion
YOD patients had higher glucose levels at diagnosis, and their glycemic control was poorly maintained. As poor glycemic control can influence the development of complications, especially in young patients, intensive treatment is necessary for patients with YOD. -
Citations
Citations to this article as recorded by- Increased risk of incident mental disorders in adults with new-onset type 1 diabetes diagnosed after the age of 19: A nationwide cohort study
Seohyun Kim, Gyuri Kim, So Hyun Cho, Rosa Oh, Ji Yoon Kim, You-Bin Lee, Sang-Man Jin, Kyu Yeon Hur, Jae Hyeon Kim
Diabetes & Metabolism.2024; 50(1): 101505. CrossRef - Association between age at diagnosis of type 2 diabetes and cardiovascular morbidity and mortality risks: A nationwide population-based study
Da Hea Seo, Mina Kim, Young Ju Suh, Yongin Cho, Seong Hee Ahn, Seongbin Hong, So Hun Kim
Diabetes Research and Clinical Practice.2024; 208: 111098. CrossRef - Impact of diabetes distress on glycemic control and diabetic complications in type 2 diabetes mellitus
Hye-Sun Park, Yongin Cho, Da Hea Seo, Seong Hee Ahn, Seongbin Hong, Young Ju Suh, Suk Chon, Jeong-Taek Woo, Sei Hyun Baik, Kwan Woo Lee, So Hun Kim
Scientific Reports.2024;[Epub] CrossRef - Early onset type 2 diabetes mellitus: an update
Myrsini Strati, Melpomeni Moustaki, Theodora Psaltopoulou, Andromachi Vryonidou, Stavroula A. Paschou
Endocrine.2024;[Epub] CrossRef - Complications and Treatment of Early-Onset Type 2 Diabetes
Fahimeh Soheilipour, Naghmeh Abbasi Kasbi, Mahshid Imankhan, Delaram Eskandari
International Journal of Endocrinology and Metabolism.2023;[Epub] CrossRef - Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
Han-sang Baek, Ji-Yeon Park, Jin Yu, Joonyub Lee, Yeoree Yang, Jeonghoon Ha, Seung Hwan Lee, Jae Hyoung Cho, Dong-Jun Lim, Hun-Sung Kim
Endocrinology and Metabolism.2022; 37(6): 945. CrossRef -
ISPAD
Clinical Practice Consensus Guidelines 2022: Management of the child, adolescent, and young adult with diabetes in limited resource settings
Anju Virmani, Stuart J. Brink, Angela Middlehurst, Fauzia Mohsin, Franco Giraudo, Archana Sarda, Sana Ajmal, Julia E. von Oettingen, Kuben Pillay, Supawadee Likitmaskul, Luis Eduardo Calliari, Maria E. Craig
Pediatric Diabetes.2022; 23(8): 1529. CrossRef - Characteristics of Glycemic Control and Long-Term Complications in Patients with Young-Onset Type 2 Diabetes (Endocrinol Metab 2022;37:641-51, Han-sang Baek et al.)
May Thu Hla Aye, Sajid Adhi Raja, Vui Heng Chong
Endocrinology and Metabolism.2022; 37(6): 943. CrossRef
- Increased risk of incident mental disorders in adults with new-onset type 1 diabetes diagnosed after the age of 19: A nationwide cohort study

- Diabetes, Obesity and Metabolism
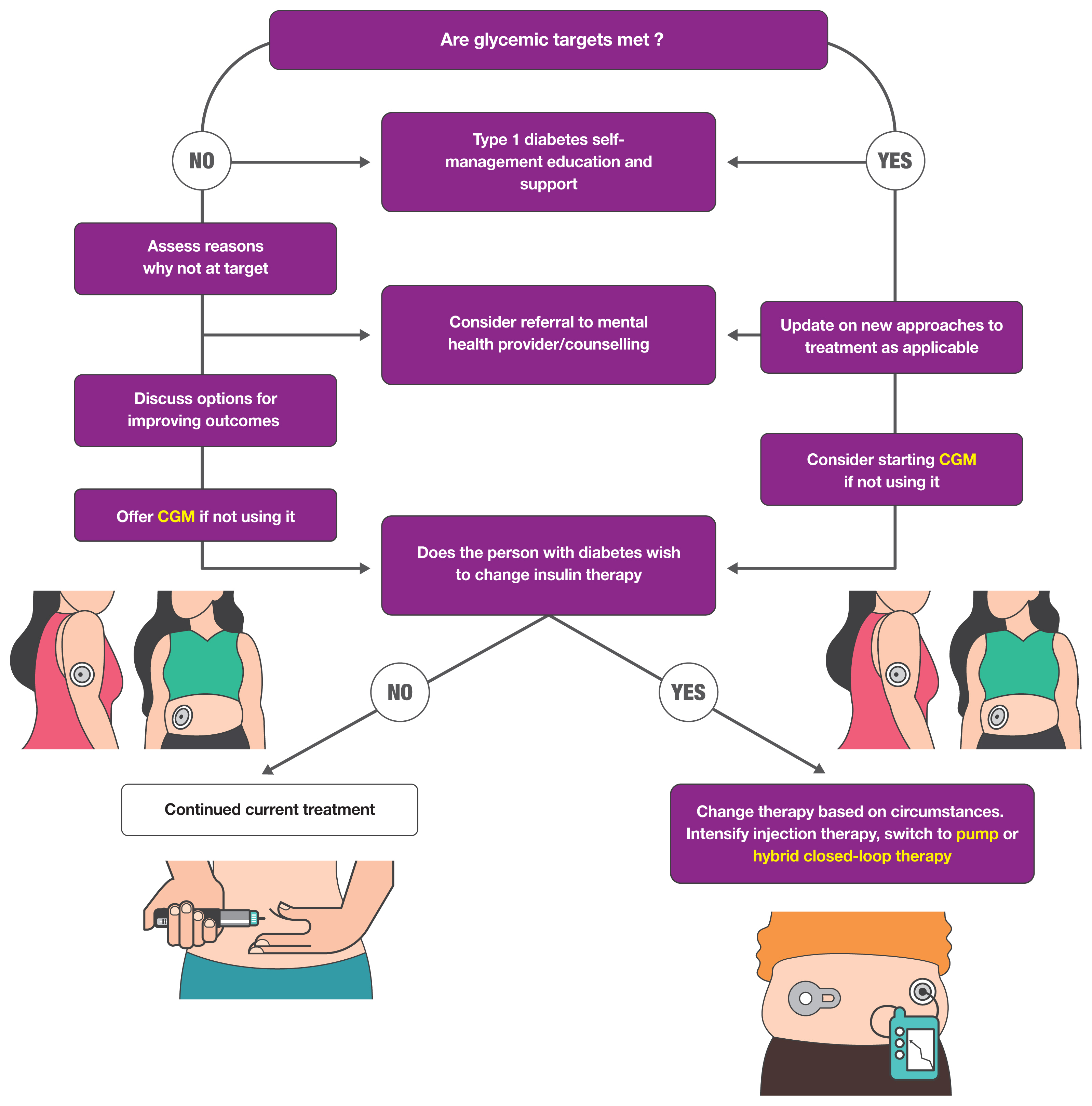
- Recent Updates to Clinical Practice Guidelines for Diabetes Mellitus
- Jin Yu, Seung-Hwan Lee, Mee Kyoung Kim
- Endocrinol Metab. 2022;37(1):26-37. Published online February 28, 2022
- DOI: https://doi.org/10.3803/EnM.2022.105
- 17,348 View
- 1,152 Download
- 22 Web of Science
- 20 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Guidelines for the management of patients with diabetes have become an important part of clinical practice that improve the quality of care and help establish evidence-based medicine in this field. With rapidly accumulating evidence on various aspects of diabetes care, including landmark clinical trials of treatment agents and newer technologies, timely updates of the guidelines capture the most current state of the field and present a consensus. As a leading academic society, the Korean Diabetes Association publishes practice guidelines biennially and the American Diabetes Association does so annually. In this review, we summarize the key changes suggested in the most recent guidelines. Some of the important updates include treatment algorithms emphasizing comorbid conditions such as atherosclerotic cardiovascular disease, heart failure, and chronic kidney disease in the selection of anti-diabetic agents; wider application of continuous glucose monitoring (CGM), insulin pump technologies and indices derived from CGM such as time in range; more active screening of subjects at high-risk of diabetes; and more detailed individualization in diabetes care. Although there are both similarities and differences among guidelines and some uncertainty remains, these updates provide a good approach for many clinical practitioners who are battling with diabetes.
-
Citations
Citations to this article as recorded by- Finerenone: Efficacy of a New Nonsteroidal Mineralocorticoid Receptor Antagonist in Treatment of Patients With Chronic Kidney Disease and Type 2 Diabetes
Subo Dey, Jasmine Garg, Andy Wang, Eva Holzner, William H. Frishman, Wilbert S. Aronow
Cardiology in Review.2024; 32(3): 285. CrossRef - Use of Diabetes Medications before and after a Heart Failure–Related Hospitalization among Nursing Home Residents
Tingting Zhang, Andrew R. Zullo, Kaleen (Kaley) N. Hayes, Dae Hyun Kim, Yoojin Lee, Lori A. Daiello, Douglas P. Kiel, Sarah D. Berry
Journal of the American Medical Directors Association.2024; 25(3): 454. CrossRef - Accuracy and Safety of the 15-Day CareSens Air Continuous Glucose Monitoring System
Kyung-Soo Kim, Seung-Hwan Lee, Won Sang Yoo, Cheol-Young Park
Diabetes Technology & Therapeutics.2024; 26(4): 222. CrossRef - Body composition and metabolic syndrome in patients with type 1 diabetes
Qiong Zeng, Xiao-Jing Chen, Yi-Ting He, Ze-Ming Ma, Yi-Xi Wu, Kun Lin
World Journal of Diabetes.2024; 15(1): 81. CrossRef - The best internal structure of the Diabetes Quality of Life Measure (DQOL) in Brazilian patients
Denilson Menezes Almeida, Aldair Darlan Santos-de-Araújo, José Mário Costa Brito Júnior, Marcela Cacere, André Pontes-Silva, Cyrene Piazera Costa, Maria Cláudia Gonçalves, José Márcio Soares Leite, Almir Vieira Dibai-Filho, Daniela Bassi-Dibai
BMC Public Health.2024;[Epub] CrossRef - Diabetes Duration, Cholesterol Levels, and Risk of Cardiovascular Diseases in Individuals With Type 2 Diabetes
Mee Kyoung Kim, Kyu Na Lee, Kyungdo Han, Seung-Hwan Lee
The Journal of Clinical Endocrinology & Metabolism.2024;[Epub] CrossRef - SGLT2 inhibitors and their possible use in prevention and treatment of neurological diseases
Mateusz Sobczyk, Daria Żuraw, Paulina Oleksa, Kacper Jasiński, Mikołaj Porzak, Michał Dacka
Prospects in Pharmaceutical Sciences.2024; 22(1): 16. CrossRef - Comparison between a tubeless, on-body automated insulin delivery system and a tubeless, on-body sensor-augmented pump in type 1 diabetes: a multicentre randomised controlled trial
Ji Yoon Kim, Sang-Man Jin, Eun Seok Kang, Soo Heon Kwak, Yeoree Yang, Jee Hee Yoo, Jae Hyun Bae, Jun Sung Moon, Chang Hee Jung, Ji Cheol Bae, Sunghwan Suh, Sun Joon Moon, Sun Ok Song, Suk Chon, Jae Hyeon Kim
Diabetologia.2024;[Epub] CrossRef - A nationwide cohort study on diabetes severity and risk of Parkinson disease
Kyungdo Han, Bongsung Kim, Seung Hwan Lee, Mee Kyoung Kim
npj Parkinson's Disease.2023;[Epub] CrossRef - Optimal Low-Density Lipoprotein Cholesterol Level for Primary Prevention in Koreans with Type 2 Diabetes Mellitus
Ji Yoon Kim, Nam Hoon Kim
Diabetes & Metabolism Journal.2023; 47(1): 42. CrossRef - Efficacy and safety of enavogliflozin versus dapagliflozin added to metformin plus gemigliptin treatment in patients with type 2 diabetes: A double-blind, randomized, comparator-active study: ENHANCE-D study
Kyung-Soo Kim, Kyung Ah Han, Tae Nyun Kim, Cheol-Young Park, Jung Hwan Park, Sang Yong Kim, Yong Hyun Kim, Kee Ho Song, Eun Seok Kang, Chul Sik Kim, Gwanpyo Koh, Jun Goo Kang, Mi Kyung Kim, Ji Min Han, Nan Hee Kim, Ji Oh Mok, Jae Hyuk Lee, Soo Lim, Sang S
Diabetes & Metabolism.2023; 49(4): 101440. CrossRef - Impact of mental disorders on the risk of heart failure among Korean patients with diabetes: a cohort study
Tae Kyung Yoo, Kyung-Do Han, Eun-Jung Rhee, Won-Young Lee
Cardiovascular Diabetology.2023;[Epub] CrossRef - Chronic disease management program applied to type 2 diabetes patients and prevention of diabetic complications: a retrospective cohort study using nationwide data
Min Kyung Hyun, Jang Won Lee, Seung-Hyun Ko
BMC Public Health.2023;[Epub] CrossRef - Innovative Therapeutic Approaches in Non-Alcoholic Fatty Liver Disease: When Knowing Your Patient Is Key
Marta Alonso-Peña, Maria Del Barrio, Ana Peleteiro-Vigil, Carolina Jimenez-Gonzalez, Alvaro Santos-Laso, Maria Teresa Arias-Loste, Paula Iruzubieta, Javier Crespo
International Journal of Molecular Sciences.2023; 24(13): 10718. CrossRef - Association between type 2 diabetes mellitus and depression among Korean midlife women: a cross-sectional analysis study
You Lee Yang, Eun-Ok Im, Yunmi Kim
BMC Nursing.2023;[Epub] CrossRef - Access to novel anti-diabetic agents in resource limited settings: A brief commentary
Poobalan Naidoo, Kiolan Naidoo, Sumanth Karamchand, Rory F Leisegang
World Journal of Diabetes.2023; 14(7): 939. CrossRef - Comparative efficacy and safety profile of once-weekly Semaglutide versus once-daily Sitagliptin as an add-on to metformin in patients with type 2 diabetes: a systematic review and meta-analysis
Tirath Patel, Fnu Nageeta, Rohab Sohail, Tooba Shaukat Butt, Shyamala Ganesan, Fnu Madhurita, Muhammad Ahmed, Mahrukh Zafar, Wirda Zafar, Mohammad Uzair Zaman, Giustino Varrassi, Mahima Khatri, Satesh Kumar
Annals of Medicine.2023;[Epub] CrossRef - Bexagliflozin, a sodium-glucose cotransporter 2 (SGLT2) inhibitor, for improvement of glycemia in type 2 diabetes mellitus: a systematic review and meta-analysis
Sagar Dholariya, Siddhartha Dutta, Ragini Singh, Deepak Parchwani, Amit Sonagra, Mehul Kaliya
Expert Opinion on Pharmacotherapy.2023; 24(18): 2187. CrossRef - Analysis of the management and therapeutic performance of diabetes mellitus employing special target
Hong-Yan Sun, Xiao-Yan Lin
World Journal of Diabetes.2023; 14(12): 1721. CrossRef - Zinc Chloride Enhances the Antioxidant Status, Improving the Functional and Structural Organic Disturbances in Streptozotocin-Induced Diabetes in Rats
Irina Claudia Anton, Liliana Mititelu-Tartau, Eliza Gratiela Popa, Mihaela Poroch, Vladimir Poroch, Ana-Maria Pelin, Liliana Lacramioara Pavel, Ilie Cristian Drochioi, Gina Eosefina Botnariu
Medicina.2022; 58(11): 1620. CrossRef
- Finerenone: Efficacy of a New Nonsteroidal Mineralocorticoid Receptor Antagonist in Treatment of Patients With Chronic Kidney Disease and Type 2 Diabetes

- Hypothalamus and Pituitary Gland
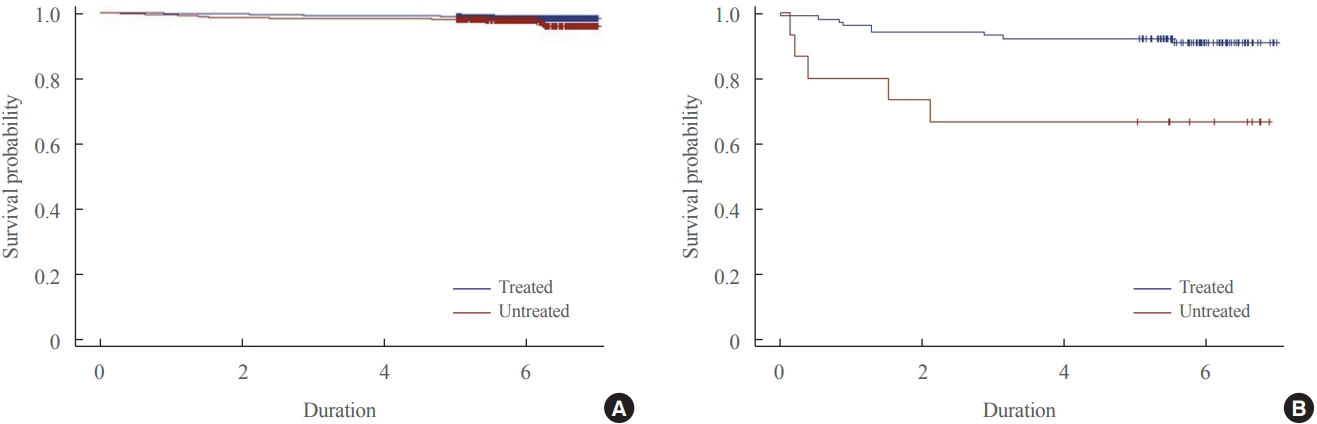
Big Data Articles (National Health Insurance Service Database) - Descriptive Epidemiology and Survival Analysis of Prolactinomas and Cushing’s Disease in Korea
- Jin Sun Park, Soo Jin Yun, Jung Kuk Lee, So Young Park, Sang Ouk Chin
- Endocrinol Metab. 2021;36(3):688-696. Published online June 28, 2021
- DOI: https://doi.org/10.3803/EnM.2021.1000
- 4,759 View
- 136 Download
- 3 Web of Science
- 3 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub - Background
Only a few studies have established the epidemiology of prolactinoma and Cushing’s disease in Korea. Furthermore, the incidence of these disease are increasing than before associated with the development of technologies. This study was designed to evaluate the epidemiology of prolactinoma and Cushing’s disease and their survival analysis according to treatment.
Methods
The nationwide, population-based study evaluated incidence and prevalence of prolactinoma and Cushing’s disease using de-identified claims data in The Korean Health Insurance Review and Assessment Service database between 2013 and 2017. The survival analysis investigated regarding treatment over a period of 6 years. A log-rank test and Cox proportional hazard regression analysis were used.
Results
The 6,056 patients with newly diagnosed prolactinoma and 584 patients with Cushing’s disease were recorded between 2013 and 2017. The annual incidence of prolactinoma was 23.5 cases per million, and its prevalence was 82.5 cases per million, and 2.3 cases per million/year and 9.8 cases per million for Cushing’s disease. The survival benefit was insignificant in prolactinoma according to treatment, but treatment of Cushing’s disease ameliorated the survival rate significantly.
Conclusion
Overall, the incidence of prolactinoma and Cushing’s disease was similar with those found previously, but the prevalence of two diseases were inconsistent when compared with the early studies. The present study also proposed necessity of treatment in Cushing’s disease for improving the survival rate. -
Citations
Citations to this article as recorded by- Big Data Research in the Field of Endocrine Diseases Using the Korean National Health Information Database
Sun Wook Cho, Jung Hee Kim, Han Seok Choi, Hwa Young Ahn, Mee Kyoung Kim, Eun Jung Rhee
Endocrinology and Metabolism.2023; 38(1): 10. CrossRef - Cushing Syndrome
Martin Reincke, Maria Fleseriu
JAMA.2023; 330(2): 170. CrossRef - Clinical Biology of the Pituitary Adenoma
Shlomo Melmed, Ursula B Kaiser, M Beatriz Lopes, Jerome Bertherat, Luis V Syro, Gerald Raverot, Martin Reincke, Gudmundur Johannsson, Albert Beckers, Maria Fleseriu, Andrea Giustina, John A H Wass, Ken K Y Ho
Endocrine Reviews.2022; 43(6): 1003. CrossRef
- Big Data Research in the Field of Endocrine Diseases Using the Korean National Health Information Database

- Clinical Study
- Comparison of Natural Course between Thyroid Cancer Nodules and Thyroid Benign Nodules
- Kyun-Jin Yun, Jeonghoon Ha, Min-Hee Kim, Ye Young Seo, Mee Kyoung Kim, Hyuk-Sang Kwon, Ki-Ho Song, Moo Il Kang, Ki-Hyun Baek
- Endocrinol Metab. 2019;34(2):195-202. Published online June 24, 2019
- DOI: https://doi.org/10.3803/EnM.2019.34.2.195
- 4,535 View
- 65 Download
- 8 Web of Science
- 8 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader  ePub
ePub Background The natural course of thyroid cancer nodules and benign nodules is different. This study was to compare the changes in size between thyroid cancer nodules and thyroid benign nodules. The risk factors associated with the changes of thyroid cancer nodules were assessed.
Methods This study contains retrospective observational and prospective analysis. A total of 113 patients with 120 nodules were recruited in the cancer group, and 116 patients with 119 nodules were enrolled in the benign group. Thyroid ultrasonography was performed at least two times at more than 1-year interval.
Results The mean follow-up durations were 29.5±18.8 months (cancer group) and 31.9±15.8 months (benign group) (
P =0.32). The maximum diameter change in length was 0.36±0.97 mm/year in the cancer group and –0.04±0.77 mm/year in the benign group (P <0.01). The volume was significantly increased in the cancer group compared with the benign group (0.06±0.18 mL/year vs. 0.004±0.05 mL/year, respectively,P <0.01; 26.9%±57.9%/year vs. 1.7%±26.0%/year,P <0.01). Initial maximum diameter (β=0.02,P <0.01) and initial volume (β=0.13,P <0.01) were significantly associated with volume change (mL)/year. Initial maximum standardized uptake value did not predict the nodule growth.Conclusion It is suggested that thyroid cancer nodules progress rapidly compared with benign nodules. Initial size and volume of nodule were independent risk factors for cancer nodule growth.
-
Citations
Citations to this article as recorded by- RAS-Mutated Cytologically Indeterminate Thyroid Nodules: Prevalence of Malignancy and Behavior Under Active Surveillance
Hannah J. Sfreddo, Elizabeth S. Koh, Karena Zhao, Christina E. Swartzwelder, Brian R. Untch, Jennifer L. Marti, Benjamin R. Roman, Jared Dublin, Ronald S. Wang, Rong Xia, Jean-Marc Cohen, Bin Xu, Ronald Ghossein, Babak Givi, Jay O. Boyle, R. Michael Tuttl
Thyroid®.2024;[Epub] CrossRef - Ultrasound for the assessment of thyroid nodules: an overview for non-radiologists
Conor Hamill, Peter Ellis, Philip C Johnston
British Journal of Hospital Medicine.2022; 83(7): 1. CrossRef - Цитологічно підтверджений вузловий зоб у членів Українсько-Американського когортного дослідження: дескриптивний аналіз результатів обстеження за 1998- 2015 роки
M.D. Tronko, L.S. Strafun, H.M. Terekhova, H.A. Zamotayeva, I.P. Pasteur
Endokrynologia.2022; 27(1): 5. CrossRef - A Computational Study on the Role of Parameters for Identification of Thyroid Nodules by Infrared Images (and Comparison with Real Data)
José R. González, Charbel Damião, Maira Moran, Cristina A. Pantaleão, Rubens A. Cruz, Giovanna A. Balarini, Aura Conci
Sensors.2021; 21(13): 4459. CrossRef - Ultrasound in active surveillance for low-risk papillary thyroid cancer: imaging considerations in case selection and disease surveillance
Sangeet Ghai, Ciara O’Brien, David P. Goldstein, Anna M. Sawka, Lorne Rotstein, Dale Brown, John de Almeida, Patrick Gullane, Ralph Gilbert, Douglas Chepeha, Jonathan Irish, Jesse Pasternak, Shereen Ezzat, James P. Brierley, Richard W. Tsang, Eric Monteir
Insights into Imaging.2021;[Epub] CrossRef - Association between various thyroid gland diseases, TSH values and thyroid cancer: a case–control study
Leif Schiffmann, Karel Kostev, Matthias Kalder
Journal of Cancer Research and Clinical Oncology.2020; 146(11): 2989. CrossRef - Combination of peroxisome proliferator–activated receptor gamma and retinoid X receptor agonists induces sodium/iodide symporter expression and inhibits cell growth of human thyroid cancer cells
Jui-Yu Chen, Jane-Jen Wang, Hsin-Chen Lee, Chin-Wen Chi, Chen-Hsen Lee, Yi-Chiung Hsu
Journal of the Chinese Medical Association.2020; 83(10): 923. CrossRef - Growth rates of malignant and benign thyroid nodules in an ultrasound follow-up study: a retrospective cohort study
Michael Cordes, Theresa Ida Götz, Karen Horstrup, Torsten Kuwert, Christian Schmidkonz
BMC Cancer.2019;[Epub] CrossRef
- RAS-Mutated Cytologically Indeterminate Thyroid Nodules: Prevalence of Malignancy and Behavior Under Active Surveillance

- Thyroid
- Accelerated Disease Progression after Discontinuation of Sorafenib in a Patient with Metastatic Papillary Thyroid Cancer
- Kyung-Jin Yun, Woohyeon Kim, Eun Hee Kim, Min-Hee Kim, Dong-Jun Lim, Moo-Il Kang, Bong-Yun Cha
- Endocrinol Metab. 2014;29(3):388-393. Published online September 25, 2014
- DOI: https://doi.org/10.3803/EnM.2014.29.3.388
- 3,579 View
- 30 Download
- 23 Web of Science
- 22 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Distant metastases from papillary thyroid carcinoma (PTC) are rare and are associated with a poor prognosis. Here, we describe a patient with metastatic PTC who was treated with a tyrosine kinase inhibitor (TKI, sorafenib) for several months that was acutely exacerbated by discontinuation. A 43-year-old male was diagnosed with PTC in February 2004 and underwent total thyroidectomy followed by two courses of high-dose radioactive iodine (RAI) therapy. Despite two additional courses of high-dose RAI therapy, lung and muscle metastases were developed. Treatment with sorafenib was begun in September 2010. After 11 months treatment of sorafenib, newly developed metastatic lesions were found in mediastinal lymph nodes, liver, and bones. Considered as treatment failure, the administration of sorafenib was discontinued. Two weeks after sorafenib treatment was stopped, the disease progressed abruptly and caused death of the patient by respiratory failure. In our patient, PTC progressed rapidly after the cessation of sorafenib treatment. Patients with several other types of cancer have also experienced such rapid disease progression, termed "flare-ups." Physicians should be aware that flare-ups may occur in advanced PTC patients following the cessation of TKI therapy.
-
Citations
Citations to this article as recorded by- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer
Silvia Martina Ferrari, Giusy Elia, Francesca Ragusa, Sabrina Rosaria Paparo, Valeria Mazzi, Mario Miccoli, Maria Rosaria Galdiero, Gilda Varricchi, Rudy Foddis, Giovanni Guglielmi, Claudio Spinelli, Concettina La Motta, Salvatore Benvenga, Alessandro Ant
Expert Opinion on Investigational Drugs.2021; 30(9): 913. CrossRef - Low Dose of Lenvatinib Treatment for Patients of Radioiodine-Refractory Differentiated Thyroid Carcinoma – A Real-World Experience
He-Jiun Jiang, Yen-Hsiang Chang, Yen-Hao Chen, Che-Wei Wu, Pei-Wen Wang, Pi-Jung Hsiao
Cancer Management and Research.2021; Volume 13: 7139. CrossRef - Rapid disease progression after discontinuation of lenvatinib in thyroid cancer
Haruhiko Yamazaki, Kiminori Sugino, Kenichi Matsuzu, Chie Masaki, Junko Akaishi, Kiyomi Hames, Chisato Tomoda, Akifumi Suzuki, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Munetaka Masuda, Koichi Ito
Medicine.2020; 99(11): e19408. CrossRef - Lenvatinib for thyroid cancer treatment: discovery, pre-clinical development and clinical application
Rosa Maria Paragliola, Andrea Corsello, Valeria Del Gatto, Giampaolo Papi, Alfredo Pontecorvi, Salvatore Maria Corsello
Expert Opinion on Drug Discovery.2020; 15(1): 11. CrossRef - Efficacy and Limitations of Lenvatinib Therapy for Radioiodine-Refractory Differentiated Thyroid Cancer: Real-World Experiences
Chie Masaki, Kiminori Sugino, Naoko Saito, Junko Akaishi, Kiyomi Y. Hames, Chisato Tomoda, Akifumi Suzuki, Kenichi Matsuzu, Takashi Uruno, Keiko Ohkuwa, Wataru Kitagawa, Mitsuji Nagahama, Koichi Ito
Thyroid.2020; 30(2): 214. CrossRef - Papillary thyroid carcinoma with hyperthyroidism and multiple metastases
Li-li Zhang, Bin Liu, Fang-fang Sun, Hong-yu Li, Shuang Li, Li-rong Zhao
Medicine.2020; 99(30): e21346. CrossRef - Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma
Leszek Herbowski
Diagnostics.2020; 10(7): 457. CrossRef - Reply to “Missing Skeletal Muscle Metastases of Papillary Thyroid Carcinoma”
Liviu Hitu, Calin Cainap, Dragos Apostu, Katalin Gabora, Eduard-Alexandru Bonci, Marius Badan, Alexandru Mester, Andra Piciu
Diagnostics.2020; 10(7): 458. CrossRef - Hif-1α Inhibitors Could Successfully Inhibit the Progression of Differentiated Thyroid Cancer in Vitro
Min-Hee Kim, Tae Hyeong Lee, Jin Soo Lee, Dong-Jun Lim, Peter Chang-Whan Lee
Pharmaceuticals.2020; 13(9): 208. CrossRef - Extended Real-World Observation of Patients Treated with Sorafenib for Radioactive Iodine-Refractory Differentiated Thyroid Carcinoma and Impact of Lenvatinib Salvage Treatment: A Korean Multicenter Study
Hye-Seon Oh, Dong Yeob Shin, Mijin Kim, So Young Park, Tae Hyuk Kim, Bo Hyun Kim, Eui Young Kim, Won Bae Kim, Jae Hoon Chung, Young Kee Shong, Dong Jun Lim, Won Gu Kim
Thyroid.2019; 29(12): 1804. CrossRef - Rapid pleural effusion after discontinuation of lenvatinib in a patient with pleural metastasis from thyroid cancer
Taisuke Uchida, Hideki Yamaguchi, Kazuhiro Nagamine, Tadato Yonekawa, Eriko Nakamura, Nobuhiro Shibata, Fumiaki Kawano, Yujiro Asada, Masamitsu Nakazato
Endocrinology, Diabetes & Metabolism Case Reports.2019;[Epub] CrossRef - Thyroid Disorders in the Elderly
Kevin Higgins
Clinics in Geriatric Medicine.2018; 34(2): 259. CrossRef - Treatment of refractory thyroid cancer
Amandine Berdelou, Livia Lamartina, Michele Klain, Sophie Leboulleux, Martin Schlumberger, _ _
Endocrine-Related Cancer.2018; 25(4): R209. CrossRef - Clinical guidance for radioiodine refractory differentiated thyroid cancer
Matti L. Gild, Duncan J. Topliss, Diana Learoyd, Francis Parnis, Jeanne Tie, Brett Hughes, John P. Walsh, Donald S.A. McLeod, Roderick J. Clifton‐Bligh, Bruce G. Robinson
Clinical Endocrinology.2018; 88(4): 529. CrossRef - Case for Stopping Targeted Therapy When Lung Cancer Progresses on Treatment in Hospice-Eligible Patients
Thomas J. Smith, Nasser Hanna, David Johnson, Sherman Baker, William A. Biermann, Julie Brahmer, Peter M. Ellis, Giuseppe Giaccone, Paul J. Hesketh, Ishmael Jaiyesimi, Natasha B. Leighl, Gregory J. Riely, Joan H. Schiller, Bryan J. Schneider, Joan Tashbar
Journal of Oncology Practice.2017; 13(12): 780. CrossRef - Intermittent Dosing of Dabrafenib and Trametinib in Metastatic BRAFV600E Mutated Papillary Thyroid Cancer: Two Case Reports
Paul S. White, Anita Pudusseri, Stephanie L. Lee, Omar Eton
Thyroid.2017; 27(9): 1201. CrossRef - Aggressive differentiated thyroid cancer with multiple metastases and NRAS and TERT promoter mutations: A case report
Fabiana Pani, Elisabetta Macerola, Fulvio Basolo, Francesco Boi, Mario Scartozzi, Stefano Mariotti
Oncology Letters.2017; 14(2): 2186. CrossRef - Tumors Sharply Increased after Ceasing Pazopanib Therapy for a Patient with Advanced Uterine Leiomyosarcoma: Experience of Tumor Flare
Terumi Tanigawa, Shintaro Morisaki, Hisanobu Fukuda, Shuichiro Yoshimura, Hisayoshi Nakajima, Kohei Kotera
Case Reports in Obstetrics and Gynecology.2017; 2017: 1. CrossRef - Initial Size of Metastatic Lesions Is Best Prognostic Factor in Patients with Metastatic Differentiated Thyroid Carcinoma Confined to the Lung
Mijin Kim, Won Gu Kim, Suyeon Park, Hyemi Kwon, Min Ji Jeon, Jong Jin Lee, Jin-Sook Ryu, Tae Yong Kim, Young Kee Shong, Won Bae Kim
Thyroid.2017; 27(1): 49. CrossRef - Articles in 'Endocrinology and Metabolism' in 2014
Won-Young Lee
Endocrinology and Metabolism.2015; 30(1): 47. CrossRef - Pharmacodynamic study of axitinib in patients with advanced malignancies assessed with 18F-3′deoxy-3′fluoro-l-thymidine positron emission tomography/computed tomography
Justine Yang Bruce, Peter Colin Scully, Lakeesha L. Carmichael, Jens C. Eickhoff, Scott B. Perlman, Jill Marie Kolesar, Jennifer L. Heideman, Robert Jeraj, Glenn Liu
Cancer Chemotherapy and Pharmacology.2015; 76(1): 187. CrossRef - Optimal Differentiated Thyroid Cancer Management in the Elderly
Donald S. A. McLeod, Kelly Carruthers, Dev A. S. Kevat
Drugs & Aging.2015; 32(4): 283. CrossRef
- Lenvatinib: an investigational agent for the treatment of differentiated thyroid cancer

- Non-functional Pituitary Adenoma Detected on (18)F-fluorodeoxyglucose Positron Emission Tomography ((18)F-FDG-PET) in a Patient with Mucosa-associated Lymphoid Tissue Lymphoma.
- Jin Ha Lee, Seung Jin Han, Se Eun Park, Mi Ae Cho, June Won Cheong, Mijin Yun, Yumie Rhee, Eun Jig Lee, Sung Kil Lim
- J Korean Endocr Soc. 2008;23(2):137-141. Published online April 1, 2008
- DOI: https://doi.org/10.3803/jkes.2008.23.2.137
- 1,830 View
- 19 Download
- 1 Crossref
-
 Abstract
Abstract
 PDF
PDF - Magnetic resonance imaging (MRI) is the modality of choice for the detection and characterization of a pituitary adenoma. Uptake of (18)F-fluorodeoxyglucose (FDG) by intrasellar tumors, including pituitary adenomas, has been reported in several previous studies. We report a case where a pituitary adenoma was detected on FDG-positron emission tomography (PET), but the tumor was not detected with the use of sellar MRI. A 31-year-old woman was referred to the clinic due to a focal increase of FDG uptake at the pituitary fossa seen on whole body FDG-PET. The patient was receiving chemotherapy due to a recurred B-cell lymphoma of the mucosa-associated lymphoid tissue type. Subsequently, sellar MRI was performed, and images showed a small non-enhancing heterogenous cystic lesion in the midline of the pituitary gland, radiologically suggestive of a Rathke's cleft cyst. However, sellar MRI failed to identify a lesion consistent with a pituitary tumor that corresponded to the site of increased FDG uptake detected by the use of PET, despite the inclusion of a dynamic contrast enhanced sequence. Despite the negative findings of the MRI examination, basal and stimulated levels of the GnRH free alpha-subunit were profoundly increased. Therefore, we suspected the presence of a non-functional pituitary tumor in addition to a Rathke's cleft cyst, rather than pituitary involvement of a lymphoma, based on the hormone levels and PET scan findings.
-
Citations
Citations to this article as recorded by- Clinical Characteristics of 16 Patients with Pituitary Tumor Incidentally Detected by18F-Fluorodeoxyglucose PET-CT (18F-FDG PET-CT)
Hyung Jin Kim, Gi Jeong Cheon, A Ra Cho, Chang Hoon Lee, Sang Min Youn, Se jin Ahn, Sang Eon Jang, Jung Min Kim, Yun Yong Lee, Ka Hee Yi
Endocrinology and Metabolism.2010; 25(4): 321. CrossRef
- Clinical Characteristics of 16 Patients with Pituitary Tumor Incidentally Detected by18F-Fluorodeoxyglucose PET-CT (18F-FDG PET-CT)

- Transcriptional Regulation of the Estrogen Receptor alpha Gene by Testosterone in Cultures of Primary Rat Sertoli Cells.
- Sang Kuk Yang, Kyung Ah Yoon, Eun Jin Yun, Kyoung Sub Song, Jong Seok Kim, Young Rae Kim, Jong Il Park, Seung Kiel Park, Byung Doo Hwang, Kyu Lim
- J Korean Endocr Soc. 2006;21(2):106-115. Published online April 1, 2006
- DOI: https://doi.org/10.3803/jkes.2006.21.2.106
- 1,653 View
- 23 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
We wanted to identify the presence of the estrogen receptor (ER) alpha in Sertoli cells and gain insight on the regulation of the ER alpha gene expression by testosterone in Sertoli cells. The transcriptional regulation of the ER alpha gene was investigated in primary Sertoli cell cultures by in situ hybridization and reverse transcription-polymerase chain reaction (RT-PCR). METHODS: Primary Sertoli cell culture was performed. The expression levels of ER alpha and ER beta mRNA in Sertoli cells were detected by Northern blot, RT-PCR, immunocytochemistry and in situ hybridization. RESULTS: The ovary, testis and epididymis showed a moderate to high expression of ER alpha while the prostate, ovary and LNCap cells showed the ER beta expression. ER alpha mRNA and protein were detected in the germ cells and Sertoli cells by in situ hybridization and immunocytochemistry. The level of ER alpha mRNA was gradually decreased in a time-dependent manner after testosterone treatment, and the changes of ER alpha mRNA were dependent on the concentration of testosterone. Androgen binding protein and testosterone-repressive prostate message-2 (TRPM-2) mRNA were reduced at 24 hour by estradiol, while the transferrin mRNA was not affected. ER alpha mRNA was strongly detectable in the testes of 7 days-old-rats, but it was gradually decreased from 14 to 21 days of age. The primary Sertoli cells also showed the same pattern. The ER alpha gene expression was also regulated by testosterone in the Sertoli cells prepared from the 14- and 21-day old rats. CONCLUSIONS: These results suggest that ER alpha is transcriptionally regulated by testosterone and it may play some role in the Sertoli cells.

- Mechanism of Castration-induced Apoptosis of Ventral Prostate in Rat.
- Chung Park, Jong Il Park, Eun Jin Yun, Kyoung Sub Song, Jong Seok Kim, Young Rae Kim, Sang Do Lee, Seung Keil Park, Byung Doo Hwang, Kyu Lim
- J Korean Endocr Soc. 2005;20(3):230-241. Published online June 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.3.230
- 1,518 View
- 20 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
S: Castration-induced androgen deprivation triggers a sequence of events, which activates apoptotic cell death of the androgen-dependent epithelial cells within the rat ventral prostate. To investigate the mechanism of castration-dependent apoptosis in the rat ventral prostate, the regulation of apoptosis-related genes was been investigated. METHODS: Azaline B was subcutaneously injected into Sprague-Dawley rat. The Fas receptor (Fas), Fas ligand (FasL) and bcl-2 mRNA, as well as the protein levels were detected by RT-PCR and Western blot analyses. Azaline B-dependent apoptosis was determined using TUNEL and a DNA fragmentation assay. The transacting factor of the FasL promoter was identified by DNA footprinting and a DNA mobility shift assay. RESULTS: The rat prostate was regressed after castration, with and the involuted ventral prostate regenerated by testosterone pretreatment, but not by that with FSH. Apoptosis of the ventral prostate was detected, after castration, using toluidine blue staining, a TUNEL assay and an apoptotic DNA fragmentation assay. The levels of Fas, FasL mRNA and protein were increased after castration. In the DNase I footprinting assay, using the FasL promoter and a nuclear extract prepared from a control prostate, at least two sites were protected: the SP-1 binding site at -283 bp and the prostate-unidentified factor(P-UF) binding site at -247 bp. The SP-1 binding activity vanished in the nuclear extract prepared from castrated rats. In the DNA mobility shift assay, the SP-1 binding activity was slightly decreased after castration. Both the Bcl-2 mRNA and Bcl-2 protein were downregulated after castration. CONCLUSION: These results suggest that the Fas/FasL system and Bcl-2 may be important to castrationdependent apoptosis in the rat ventral prostate, with SP-1 related to the castration-dependent regulation of the FasL gene

- A Case of Licorice Induced Hypokalemic Paralysis with Rhabdomyolysis.
- Hyun Il Hong, Koon Hee Han, Jung Won Hwang, Young Don Kim, Myung Sook Shim, Jin Yub Kim
- J Korean Endocr Soc. 2005;20(2):179-182. Published online April 1, 2005
- DOI: https://doi.org/10.3803/jkes.2005.20.2.179
- 1,740 View
- 19 Download
- 4 Crossref
-
 Abstract
Abstract
 PDF
PDF - Prolonged ingestion of licorice can cause hypermineralocorticoidism, with sodium retention, potassium loss and hypertension. Nevertheless, its initial presentation with a very severe degree of hypokalemic paralysis and rhabdomyolysis are exceedingly rare. We describe a patient who experienced hypokalemic paralysis and rhabdomyolysis after licorice ingestion. The patient's initial blood pressure was 160/80mmHg. The major biochemical abnormalities included; hypokalemia(K+ 1.3mEq/L), metabolic alkalosis, with a pH of 7.64, and urine myoglobin > 3000ng/mL. The plasma rennin activity and aldosterone level were suppressed. The 24 hour urine cortisol concentration was normal. The patients, over a 1 month period, had ingested 500g of licorice boiled in water. After quitting the licorice, the hypokalemia and muscle paralysis gradually improved and blood pressure returned to normal
-
Citations
Citations to this article as recorded by- A case of chronic licorice intoxication-induced apparent mineralocorticoid excess syndrome
Young Jae Lim, Ji Eun Kim
Journal of The Korean Society of Clinical Toxicology.2023; 21(2): 151. CrossRef - Hypokalemic Periodic Paralysis Developed in a Patient with Neurogenic Diabetes Insipidus
Jihyeon Hwang, Joo Hye Sung, Ye Eun Kim, Keonyeup Kim, Seong-Hwan Kim, Young Bin Park, Seol-Hee Baek
Journal of the Korean Neurological Association.2021; 39(3): 177. CrossRef - Electrical storm induced by hypokalemia associated with herbal medicines containing licorice
Hyun Kuk Kim, Sung Soo Kim
Translational and Clinical Pharmacology.2019; 27(2): 69. CrossRef - Influence of Herbal Complexes Containing Licorice on Potassium Levels: A Retrospective Study
WooSang Jung, SeungWon Kwon, JinWook Im, SeongUk Park, SangKwan Moon, JungMi Park, ChangNam Ko, KiHo Cho
Evidence-Based Complementary and Alternative Medicine.2014; 2014: 1. CrossRef
- A case of chronic licorice intoxication-induced apparent mineralocorticoid excess syndrome

- Specialized Functions and Hormonal Regulation of Sertoli Cell.
- Kyu Lim, Chung Park, Kyung Ah Yun, Eun Jin Yun, Jong Il Park, Seung Kiel Park, Byung Doo Hwang
- J Korean Endocr Soc. 2003;18(2):120-136. Published online April 1, 2003
- 978 View
- 16 Download

- Effect of Radioactive Iodine Therapy in Patients with Scan-Negative, Thyroglobulin-Positive Thyroid Cancer.
- Eun Sook Kim, Seok Jun Hong, Jin Yub Kim, Young Ki Song, Jin Sook Ryu, Dae Hyuk Moon, Ki Soo Kim, Sang Wook Kim
- J Korean Endocr Soc. 1999;14(2):330-338. Published online January 1, 2001
- 1,148 View
- 22 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
After total thyroidectomy the presence of detectable serum thyroglobulin(Tg) concentration is an index of residual or metastatic thyroid tissue and is usually well correlated with positive I whole body scan. However, it is not rare to find a patient with detectable serum Tg levels but without any uptake on I whole-body scan. At present it is not certain how to manage such patients. We performed whole body scan after administration of therapeutic dose of 131I to evaluate the usefulness of radioactive iodine therapy in the above setting. METHODS: Fifteen patients (4 males and 11 females, ranging in age from 17 to 74 years) were studied. They had been previously treated with total thyroidectomy for papillary thyroid cancer followed by therapy with 131I for ablation of their thyroid residue. Tg levels were determined by immunoradiometric assay method. 131I (100-200 mCi) therapy was administered and whole body scan was performed. 99mTc MIBI scans were taken in 9 patients. Follow up data of Tg were available in 12 patients at time interval of 6 12 months from the first study and treatment. RESULTS: Tg(on) levels of these patients were in a range of 2.2210 ng/mL (mean 36.1 +/- 59.1 ng/mL) and Tg(off) levels were 17.3 1,592 ng/mL (mean 197.3 +/- 400.3 ng/mL). After radioiodide therapy, Tg(on) levels were in 1.48.5 ng/mL (mean 11.0 +/- 13.5 ng/mL), Tg (off) were 11.9 478.0 ng/mL (mean 159.3 +/- 159.8 ng/mL). The Tg (on) levels were decreased significantly after RAI therapy, but Tg (off) levels had no significant difference, In 8 of the 15 patients (53.3%), posttreatment whole body scan showed definite positive uptakes which were not evident in pretreatment diagnostic scan. There were local recurrence in 3 cases, regional lymph node metastasis in 4 cases, and lung in I case. Diffuse hepatic uptake was definitely seen in 7 cases. The MIBI scan showed abnorml uptakes in 4 of 9 cases. CONCLUSION: The therapeutic usefulness of 100 to 200 mCi of 131I treatment in patients with 131I scan-negative and Tg-positive was unclear. And the MIBI scan was only partially effective. Further studies with other diagnostic and therapeutic approachs are required to evaluate the exact lesions and to improve prognosis.


 KES
KES

 First
First Prev
Prev



